Weaver syndrome
| Weaver syndrome | |
|---|---|
 | |
| Classification and external resources | |
| Specialty | medical genetics |
| ICD-10 | Q87.3 |
| OMIM | 277590 |
Weaver syndrome (also called Weaver-Smith syndrome) is an extremely rare congenital disorder associated with rapid growth beginning in the prenatal period and continuing through the toddler and youth years. It is characterized by advanced osseous maturation, and distinctive craniofacial, skeletal, and neurological abnormalities.[1] It was first described by Dr. David Weaver in 1974.[2] It is similar to Sotos syndrome.
Signs and symptoms
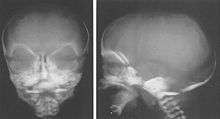
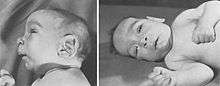
Children with Weaver syndrome tend to look similar and have distinctive physical and craniofacial characteristics, which may include several, but not all of the following features:
- Macrocephaly
- Large bifrontal diameter
- Flattened occiput
- Long philtrum
- Retrognathia
- Round face in infancy
- Prominent chin crease
- Large ears
- Strabismus
- Hypertelorism
- Epicanthal folds
- Downslanting palpebral fissures
Other features may include loose skin, thin deep-set nails, thin hair, short ribs, limited elbow and knee extension, camptodactyly, and a coarse, low-pitched voice. Delayed development of motor skills such as sitting, standing, and walking are commonly exhibited in early childhood. Patients with Weaver syndrome typically have mild intellectual disability with poor coordination and balance.[3] They also have some neurological abnormalities such as speech delay, seizures, mental retardation, hypotonia or hypertonia, and behavioral problems.
Cause
A common cause for Weaver syndrome is mutations in the EZH2 gene on chromosome 7q36.[4] EZH2 (Enhancer of Zeste, Drosophila, homolog 2), is the second histone methyltransferase associated with human overgrowth. It encodes the catalytic component of the PRC2 protein complex (Polycomb Repressive Complex 2), which regulates chromatin structure and gene expression, and has been found to repress transcription. EZH2 also has critical roles in stem cell maintenance and cell lineage determination, such as osteogenesis, myogenesis, lymphopoiesis and hematopoiesis.[5]
It can also be associated with mutations in the histone methyltransferase NSD1 gene on chromosome 5q35. The functions of NSD1 are not clearly known, but it is thought to act as a factor in influencing transcription, which contains domains involved in chromatin-mediated regulation during development.[6]
Most cases are found to be sporadic, with no family history of the syndrome, although there have been a few cases in families where autosomal dominant inheritance has been reported.[7]
Distinctions between Weaver syndrome and Sotos syndrome
Weaver syndrome and Sotos syndrome are often mistaken for one another due to their significant phenotypic overlap and similarities.[8] Clinical features shared by both syndromes include overgrowth in early development, advanced bone age, developmental delay, and prominent macrocephaly.[9] Mutations in the NSD1 gene may also be another cause for confusion. The NSD1 gene provides instructions for making a protein that is involved in normal growth and development. Deletions and mutations in the NSD1 gene is a common cause for patients with Sotos syndrome and in some cases for Weaver syndrome as well.
Features distinguishing Weaver syndrome from Sotos syndrome include broad forehead and face, ocular hypertelorism, prominent wide philtrum, micrognathia, deep-set nails, retrognathia with a prominent chin crease, increased prenatal growth, and a carpal bone age that is greatly advanced compared to metacarpal and phalangeal bone age.[10]
Treatment
There is no cure available for Weaver syndrome. However, with multidisciplinary management such as neurological, pediatric, orthopedic, and psychomotor care and genetic counseling, symptoms can be managed. Surgery may be used to correct any skeletal issues. Physical and occupational therapy are considered an option to help with muscle tone. Also, speech therapy is often recommended for speech related problems.[11]
Prognosis
With appropriate treatment and management, patients with Weaver syndrome appear to do well, both physically and intellectually, throughout their life and have a normal lifespan.[12] Their adult height is normal as well.
See also
References
- ↑ CRAWFORD, MARK W., and DENISE ROHAN. "The Upper Airway In Weaver Syndrome." Pediatric Anesthesia 15.10 (2005): 893-896. Health Source: Nursing/Academic Edition.
- ↑ Weaver DD, Graham CB, Thomas IT, Smith DW (1974). "A new overgrowth syndrome with accelerated skeletal maturation, unusual facies, and al=J. Pediatr.". 84 (4): 547–52. PMID 4366187.
- ↑ Genetics Home Reference. "Weaver syndrome". U.S. National Library of Medicine. Retrieved 9 November 2013.
- ↑ Gibson, William T; Hood Rebecca L, Zhan Shing Hei, Bulman Dennis E, Fejes Anthony P, Moore Richard, Mungall Andrew J, Eydoux Patrice, Babul-Hirji Riyana, An Jianghong, Marra Marco A, , Chitayat David, Boycott Kym M, Weaver David D, Jones Steven J M (Dec. 2011). "Mutations in EZH2 Cause Weaver Syndrome". American Journal of Human Genetics (in ENG) 90 (1): 110–8.
- ↑ Germline mutations in the oncogene EZH2 cause Weaver syndrome and increased human height Katrina Tatton-Brown, Sandra Hanks, Elise Ruark, Anna Zachariou, Silvana Del Vecchio Duarte, Emma Ramsay, Katie Snape, Anne Murray, Elizabeth R Perdeaux, Sheila Seal, Chey Loveday, Siddharth Banka, Carol Clericuzio, Frances Flinter, Alex Magee, Vivienne McConnell, Michael Patton, Wolfgang Raith, Julia Rankin, Miranda Splitt, Volker Strenger, Clare Taylor, Patricia Wheeler, I Karen Temple, Trevor Cole, The Childhood Overgrowth Collaboration, Jenny Douglas, Nazneen Rahman Oncotarget. 2011 December; 2(12): 1127–1133. Published online 2011 December 21.
- ↑ Douglas J, Hanks S, Temple IK, et al. (2003). "NSD1 mutations are the major cause of Sotos syndrome and occur in some cases of Weaver syndrome but are rare in other overgrowth phenotypes". Am. J. Hum. Genet. 72 (1): 132–43. doi:10.1086/345647. PMC 378618
 . PMID 12464997.
. PMID 12464997. - ↑ Cole, Trevor R.P., N.R. Dennis, and Helen E. Hughes. "Weaver Syndrome: Seven New Cases and a Review of the Literature." In Congenital Malformation Syndromes. New York: Chapman and Hall Medical, 1995, pp. 267-280.
- ↑ NSD1 Mutations Are the Major Cause of Sotos Syndrome and Occur in Some Cases of Weaver Syndrome but Are Rare in Other Overgrowth Phenotypes Jenny Douglas, Sandra Hanks, I. Karen Temple, Sally Davies, Alexandra Murray, Meena Upadhyaya, Susan Tomkins, Helen E. Hughes, Trevor R. P. Cole, Nazneen Rahman Am J Hum Genet. 2003 January; 72(1): 132–143. Published online 2002 December 2.
- ↑ Gibson, William T; Hood Rebecca L, Zhan Shing Hei, Bulman Dennis E, Fejes Anthony P, Moore Richard, Mungall Andrew J, Eydoux Patrice, Babul-Hirji Riyana, An Jianghong, Marra Marco A, , Chitayat David, Boycott Kym M, Weaver David D, Jones Steven J M (Dec. 2011). "Mutations in EZH2 Cause Weaver Syndrome". American Journal of Human Genetics (in ENG) 90 (1): 110–8.
- ↑ Gibson, William T; Hood Rebecca L, Zhan Shing Hei, Bulman Dennis E, Fejes Anthony P, Moore Richard, Mungall Andrew J, Eydoux Patrice, Babul-Hirji Riyana, An Jianghong, Marra Marco A, , Chitayat David, Boycott Kym M, Weaver David D, Jones Steven J M (Dec. 2011). "Mutations in EZH2 Cause Weaver Syndrome". American Journal of Human Genetics (in ENG) 90 (1): 110–8.
- ↑ Hunter, Cindy L. "Weaver syndrome". Gale Encyclopedia of Public Health. Retrieved 9 November 2013.
- ↑ Hunter, Cindy L. "Weaver syndrome". Gale Encyclopedia of Public Health. Retrieved 9 November 2013.
