Periodontal fiber
| Periodontal ligament | |
|---|---|
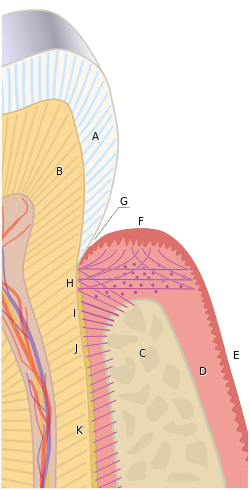 The tissues of the periodontium combine to form an active, dynamic group of tissues. The alveolar bone (C) is surrounded for the most part by the subepithelial connective tissue of the gingiva, which in turn is covered by the various characteristic gingival epithelia. The cementum overlaying the tooth root is attached to the adjacent cortical surface of the alveolar bone by the alveolar crest (I), horizontal (J) and oblique (K) fibers of the periodontal ligament. | |
| Details | |
| Precursor | dental follicle |
| Identifiers | |
| Latin | fibra periodontalis |
| FMA | 56665 |
The periodontal ligament, commonly abbreviated as the PDL, is a group of specialized connective tissue fibers that essentially attach a tooth to the alveolar bone within which it sits.[1]
Development
Similar to the alveolar bone, the PDL develops from the dental sac of the tooth germ.[2]
Features
Functions of PDL are supportive, sensory, nutritive, and remodeling.[3]
The PDL substance has been estimated to be 70% water, which is thought to have a significant effect on the tooth's ability to withstand stress loads. The completeness and vitality of the PDL are essential for the functioning of the tooth.
The PDL ranges in width from 0.15 to 0.38mm with its thinnest part located in the middle third of the root.[4]
The PDL is a part of the periodontium that provide for the attachment of the teeth to the surrounding alveolar bone by way of the cementum.
The PDL appears as the periodontal space of 0.4 to 1.5 mm on radiographs, a radiolucent area between the radiopaque lamina dura of the alveolar bone proper and the radiopaque cementum.
There are progenitor cells in the periodontal ligament that can differentiate into osteoblasts for the physiological maintenance of alveolar bone and, most likely, for its repair as well.[5]
Structure
The PDL consist of cells, and extracellular compartment of fibers.[5] The cells are fibroblast, epithelial cells, undifferentiated mesenchymal cells, bone and cementum cells. The epithelial rests of Malassez are also present; these groups of epithelial cells become located in the mature PDL after the disintegration of Hertwig epithelial root sheath during the formation of the root.[2] The extracellular compartment consists of Type 1, 3, and 5 collagen fibers bundles embedded in intercellular substance. The PDL collagen fibers are categorized according to their orientation and location along the tooth.[6]
Alveolodental ligament
The main principal fiber group is the alveolodental ligament, which consists of five fiber subgroups: alveolar crest, horizontal, oblique, apical, and interradicular on multirooted teeth. Principal fibers other than the alveolodental ligament are the transseptal fibers.
All these fibers help the tooth withstand the naturally substantial compressive forces which occur during chewing and remain embedded in the bone. The ends of the principal fibers that are within either cementum or alveolar bone proper are considered Sharpey fibers.
Alveolar crest fibers
Alveolar crest fibers (I)run from the cervical part of the root to the alveolar bone crest
Horizontal fibers
Horizontal fibers (J) attach to the cementum apical to the alveolar crest fibers and run perpendicularly from the root of the tooth to the alveolar bone.
Oblique fibers
Oblique fibers (K) are the most numerous fibers in the periodontal ligament, running from cementum in an oblique direction to insert into bone coronally.
Apical fibers
Apical fibers are found radiating from cementum around the apex of the root to the bone, forming base of the socket or alveolus.
Interradicular fibers
Interradicular fibers are only found between the roots of multirooted teeth, such as premolars and molars. They extend from radicular cementum to interradicular alveolar bone.
Transseptal fibers
Transseptal fibers (H) extend interproximally over the alveolar bone crest and are embedded in the cementum of adjacent teeth; they form an interdental ligament. These fibers keep all the teeth aligned. These fibers may be considered as belonging to the gingival tissue because they do not have an osseous attachment.[7]
Pathology
- Damage to the PDL may result in tooth ankylosis to the jawbone, making the tooth lose its continuous eruption ability. Dental trauma, such as subluxation, may cause tearing of the PDL and pain during function (eating).[8]
- The epithelial rests of Malassez can become cystic, usually forming nondiagnostic, radiolucent apical lesions that can be seen on radiographs. This occurs as a result of chronic periapical inflammation after pulpitis occurs and must be surgically removed.[2]
- The PDL also undergoes drastic changes with chronic periodontal disease that involves the deeper structures of the periodontium with periodontitis. The fibers of the PDL become disorganized, and their attachments to either the alveolar bone proper or cementum through Sharpey fibers are lost because of the resorption of these two hard dental tissue.[2]
- When traumatic forces of occlusion are placed on a tooth, the PDL widens to take the extra forces. Thus, early occlusal trauma can be viewed on radiographs as a widening of the periodontal ligament space. Thickening of the lamina dura in response is also possible. Clinically, occlusal trauma is noted by the late manifestation of increased mobility of the tooth and possibly the presence of pathological tooth migration.[2]
External links
- Max A. Listgarten, University of Pennsylvania and Temple University at http://www.dental.pitt.edu/informatics/periohistology/en/gu0401.htm
- Structure of periodontal tissues in health and disease, Nanci and Bosshardt, Periodontology 2000, Vol. 40, 2006, 11–28 at http://www.nancicalcifiedtissuegroup.com/documents/Nanci%202006.pdf
See also
References
- ↑ Herbert F. Wolf; Klaus H. Rateitschak (2005). Periodontology. Thieme. pp. 12–. ISBN 978-0-86577-902-0. Retrieved 21 June 2011.
- 1 2 3 4 5 Illustrated Dental Embryology, Histology, and Anatomy, Bath-Balogh and Fehrenbach, Elsevier, 2011, page 184.
- ↑ Max A. Listgarten, University of Pennsylvania and Temple University at http://www.dental.pitt.edu/informatics/periohistology/en/gu0401.htm
- ↑ Ten Cate's Oral Histology, Nanci, Elsevier, 2013, page 220
- 1 2 Structure of periodontal tissues in health and disease, ANTONIO NANCI & DIETER D. BOSSHARDT, Periodontology 2000, Vol. 40, 2006, 11–28 at http://www.nancicalcifiedtissuegroup.com/documents/Nanci%202006.pdf
- ↑ Max A. Listgarten, University of Pennsylvania and Temple University, http://www.dental.pitt.edu/informatics/periohistology/en/gu0404.htm
- ↑ Ten Cate's Oral Histolog, Nanci, Elsevier, 2013, page 274
- ↑ Zadik Y (December 2008). "Algorithm of first-aid management of dental trauma for medics and corpsmen". Dent Traumatol. 24 (6): 698–701. doi:10.1111/j.1600-9657.2008.00649.x. PMID 19021668.